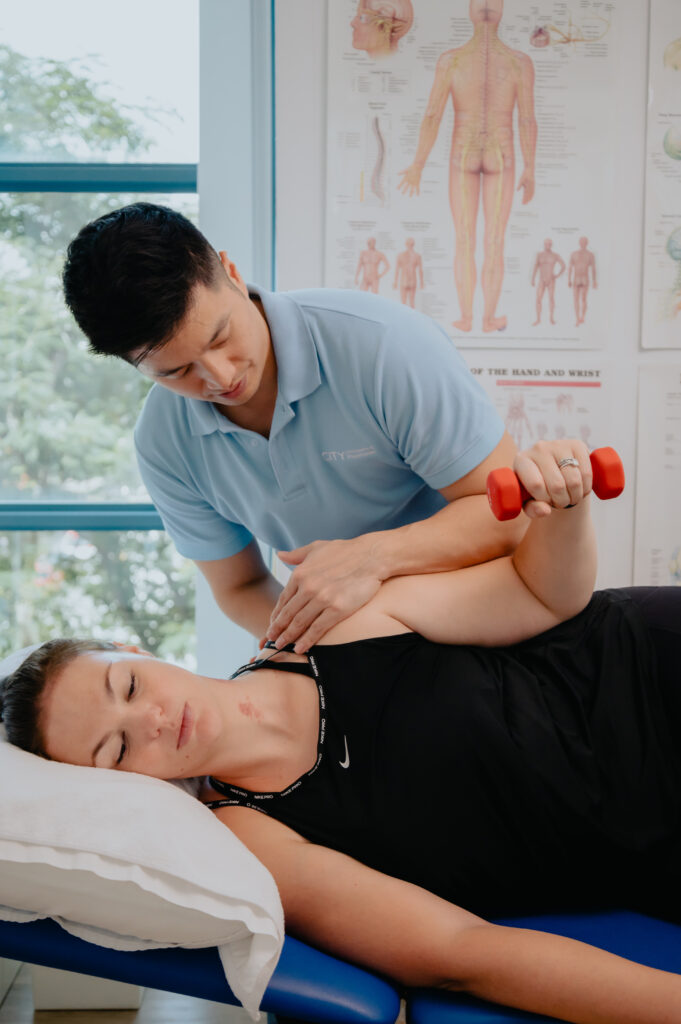
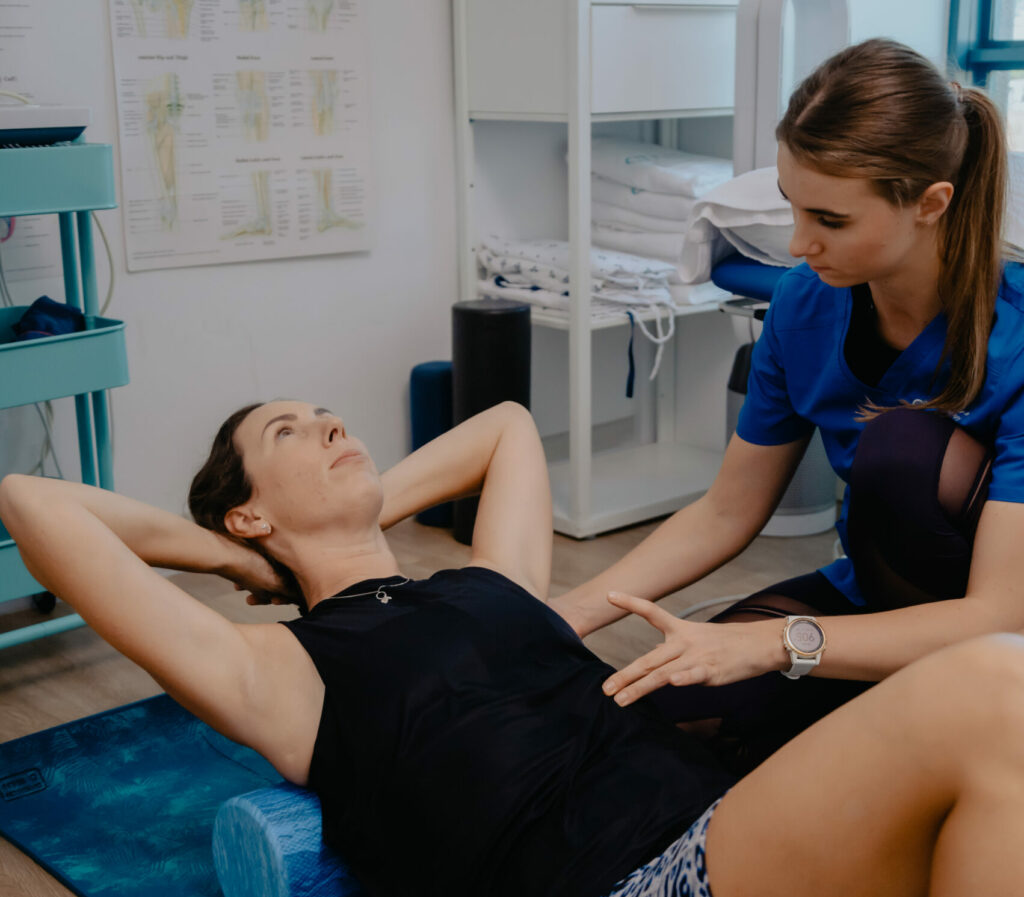
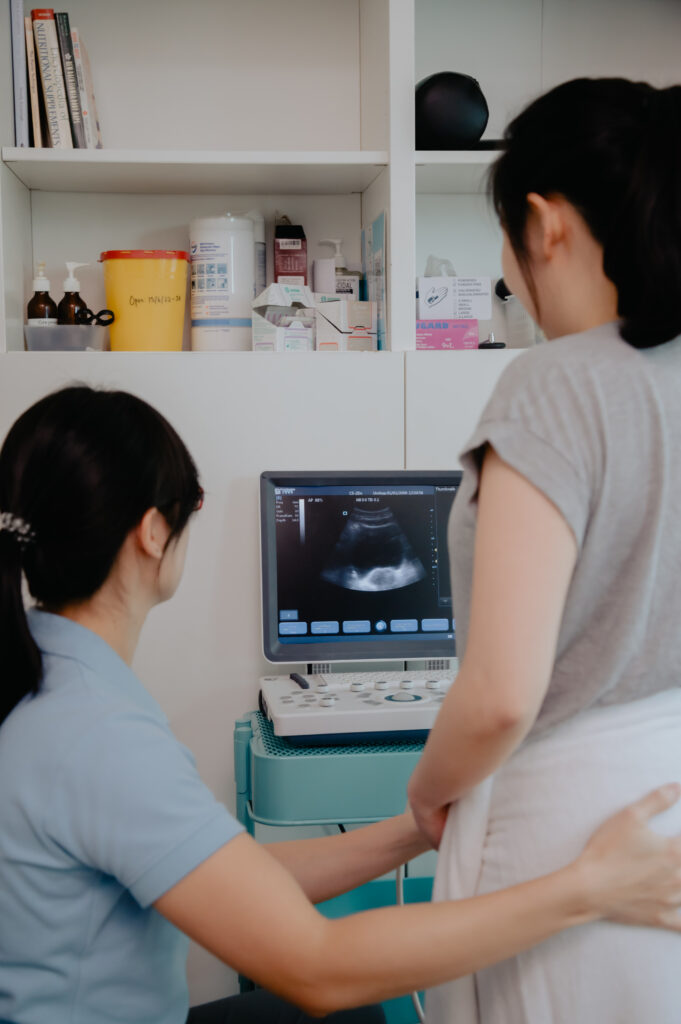
Does insurance cover paediatric sessions?
City Osteopathy and Physiotherapy offers direct billing service for several insurance providers:




To enjoy cashless transaction please bring with you:
- Membership card
- Doctor’s referral letter (if needed per your insurance policy)
- LOG – letter of guarantee (if applicable)
Don’t worry if your insurance is not listed here. After each session we will email you an itemized bill so you can submit it for reimbursement.
We do not charge for completing medical insurance forms, but an administration fee is charged if an official letter or report is required to be produced for the insurance company or other entity.
- Filling out insurance forms: Free
- Writing a letter to insurance companies: $140
- Full medical report for insurance companies or other entity: From $250